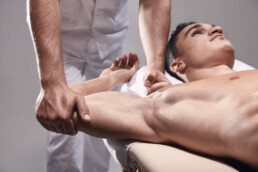
Rolfing® Structural Integration
Every body needs to know that physical health is not a luxury! Are you ready for transformation? Learn more about Rolfing® Structural Integration:
- Rolfing Structural Integration reorganizes the body through 10 sessions of client-focused interactive hands-on bodywork.
- Each session is a combination of manipulative techniques, movement cues, and client education.
- The results of Structural Integration are long lasting and are backed by scientific study.
Integrative Bodywork
Anything that is worth having requires maintenance. Your body is no different! Learn more about Integrative Bodywork and its benefits:
- Integrative Bodywork is hands-on bodywork to pinpoint and address specific problem areas.
- Perfect for routine maintenance of the body or to fix minor issues.
- Helps common conditions such as back pain, neck pain, carpal tunnel syndrome and plantar fasciitis.
Services
Rolfing® Structural Integration
Do you want to be more physically adaptable? Be able to breathe fully with ease? Have less back pain? Then Rolfing Structural Integration might be right for you.
Integrative Bodywork
Completely customized to you and your individual needs, Integrative Bodywork is the maintenance plan your body is looking for.
Massage
Make massage a part of your regular physical maintenance routine! Gift certificates and packages are available.
Ayurveda
Āyurveda’s foundational knowledge of health helps you to understand yourself in a new and approachable way.
What our clients say
Eric is a skilled and safe bodyworker. The 10-series of rolfing/structural integration eliminated my lower back pain entirely. I would highly recommend him to anyone interested in a transformative body work experience.
– Alex
After a few trips to Chattanooga Bodyworks my sciatica and back pain disappeared. He has truly been a blessing in my life.
– Jacob
The care I received from Eric seriously took about 20 years off of my body. I struggled to walk or sit comfortably. Rolfing completely released the painful muscle spasms and gave me back my flexibility and a pain-free life. I truly cannot thank Dr. Maklan enough for giving me my life back. I never would have imagined I could feel this kind of ease in my body again.
– Crystal
With the help of Rolfing sessions at Chattanooga Bodyworks, I have regained much of the natural integrity of my body’s form, enhanced my postural efficiency and regained freedom of movement Eric’s knowledge, intuition and compassion is immediately obvious.
– Veronica
I saw Eric due to a hamstring issue from running. One visit and I was able to start sprinting again.
– Randy





- Alex

- Jacob

- Crystal

- Veronica

- Randy

Our location
Contact Us
Every body needs to know that physical health is not a luxury! Are you ready for transformation?